-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 8 Issue 5
Pigment dispersion syndrome: a brief overview
Marco Zeppieri
Zeppieri et al. J Clin Transl Res 2022; 8(5):4
Published online: September 7, 2022
Abstract
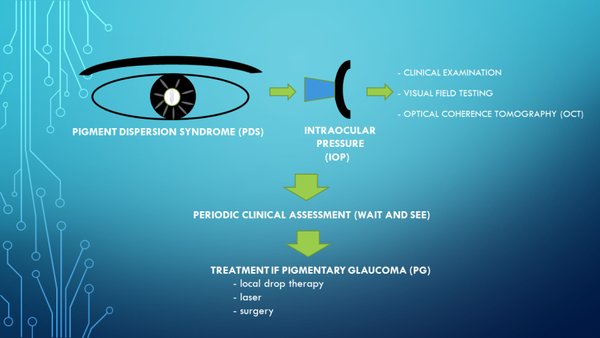
Background. Pigment dispersion syndrome (PDS) is characterized by dispersion of pigment in the anterior chamber structures and can present with deposits on the central corneal endothelium or Krukenberg spindle, iris trans-illumination spoke-like defects, and increased pigmentation in the iridocorneal angle. It is more common in myopic patients with a predominance in young males in the third to fifth decade of life that affects about 1-2% of the population. PDS is a risk factor and can give lead to a rise in intraocular pressure (IOP) and secondary glaucoma. Pigmentary glaucoma (PG) can develop from PDS in the presence of elevated IOP coupled with glaucomatous optic neuropathy, retinal nerve fiber thinning, and/or visual field defects. PDS and PG have the same clinical features, representing different levels of severity on the same clinical spectrum.
Relevance for patients. Early diagnosis, appropriate management and follow-up of patients with PDS is important to prevent vision deterioration or blindness due to glaucomatous optic neuropathy.
DOI: http://dx.doi.org/10.18053/jctres.08.202205.004
Author affiliation
Department of Ophthalmology, University Hospital of Udine, Italy
*Corresponding author
Marco Zeppieri
Department of Ophthalmology, University Hospital of Udine; p.le S. Maria della Misericordia 15, 33100 Udine, Italy
Email: markzeppieri@hotmail.com
Handling editor:
Michal Heger
Department of Pharmaceutics, Utrecht University, the Netherlands
Department of Pharmaceutics, Jiaxing University Medical College, Zhejiang, China

