-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 8 Issue 4
Systemic anti-inflammatory effects of mesenchymal stem cells in burn: A systematic review of animal studies
Abdullah S. Eldaly*, Sarah M. Mashaly, Eslam Fouda, Omar S. Emam, Amro Aglan, Jumanah Abuasbeh, Aditya Khurana, Hiba Hamdar, Ayman R. Fath
Eldaly et al. J Clin Transl Res 2022; 8(4):3
Published online: July 18, 2022
Abstract
Background: Despite the advances in burn care, severe burns still impose significant morbidity and mortality. Severe burns are associated with an inflammatory response that ranges from alterations in vital signs to shock, multiorgan failure and death.
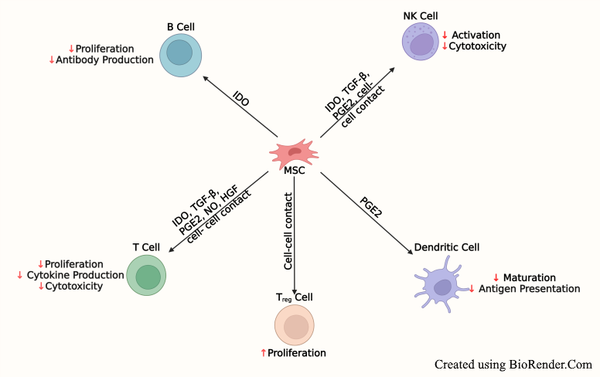
Mesenchymal stem cells (MSCs) are known for their anti-inflammatory and immunomodulatory effects. Therefore, MSCs were investigated for their potential benefits in modulating burn-induced inflammation and organ damage in several studies.
Aim: We have conducted a systematic review of literature to evaluate the efficacy of MSCs in modulating burn-induced systemic inflammation and organ damage in animal models.
Methods: Four databases were searched: PubMed, Cumulative Index of Nursing and Allied Health Literature (CINAHL), Scopus, and Web of Science. We used the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) as our basis of organization.
Results: Eight studies were included. Bone marrow derived MSCs (BMMSCs), umbilical cord derived MSCs (UC-MSCs), and UC-MSCs exosomes were used to modulate the burn-induced inflammation. MSCs therapy reduced serum levels of pro-inflammatory cytokines, improved renal fucntion, inhibited tissue damage, and improved survival after burn. Furthermore, MSCs reversed all the burn-induced pathological changes in blood brain barrier (BBB).
Conclusion: MSCs may attenuate the burn-induced inflammation by decreasing serum levels of inflammatory cytokines. However, the effect on anti-inflammatory cytokines is conflicting and mandates more substantial evidence. Furthermore, MSCs reduce tissue inflammation, tissue damage, and apoptosis in the lungs and kidneys. In addition, MSCs reversed the burn-induced pathophysiologic changes in the BBB. The underlying mechanisms of these effects are poorly understood and should be the focus of future stem cell research.
Relevance to patients: Severe burn patients are liable to systemic inflammation due to the release of inflammatory cytokines into the circulation. This inflammatory response has a broad spectrum of severity that ranges from alterations in vital signs to multiorgan failure and death. Despite the advances in burn care, burn-induced inflammation still imposes significant morbidity and mortality. This systematic review evaluates the potential benefits of stem cells in modulating burn-induced systemic inflammation in animal burn models.
DOI: http://dx.doi.org/10.18053/jctres.08.202204.003
Author affiliation
1. Division of Plastic Surgery, Mayo Clinic, Jacksonville, Florida.
2. Dermatology Department, El-Menshawy General Hospital, Tanta, Egypt.
3. Division of Anesthesia and Perioperative Medicine, Mayo Clinic, Jacksonville, Florida.
4. Internal Medicine Department, Lahey Clinic Beth Israel, Boston, Massachusetts.
5. Public Health Department, University of Arizona, Phoenix, Arizona.
6. Internal Medicine Department, Creighton University Health Education Alliance, Phoenix, Arizona.
7. Emergency Medicine Department, Notre Dame Maritime Hospital, Byblos, Lebanon
*Corresponding Author
Abdullah S. Eldaly
Division of Plastic Surgery, Mayo Clinic, 4500 San Pablo Rd, Jacksonville, FL
32224
Tel: +1 9045974771
Email: abdullaheldali@gmail.com
Handling editor:
Michal Heger
Department of Pharmaceutics, Utrecht University, the Netherlands
Department of Pharmaceutics, Jiaxing University Medical College, Zhejiang, China

