-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 8 Issue 2
Inactivated COVID-19 vaccine triggering hemophagocytic lymphohistiocytosis in an immunocompetent adult - A case report
Saad Nasir, Saqib Raza Khan*, Rodaba Iqbal, Alizah Pervaiz Hashmi, Munira Moosajee, Noreen Nasir
Nasir et al. J Clin Transl Res 2022; 8(1):9
Published online: March 31, 2022
Abstract
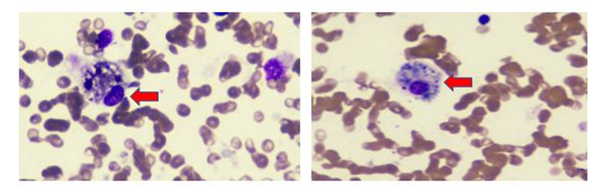
Background and aim: Hemophagocytic lymphohistiocytosis (HLH) is a severe hyperinflammatory syndrome that is induced by hyper-activated macrophages, cytotoxic T cells, and reduced natural killer (NK) cell activity. A 46-year-old gentleman presented to us with complaints of intermittent fever for the past two weeks associated with fatigue along with oral ulcers and skin rashes which resolved spontaneously. These symptoms started after he received the second dose of the BBIP-CorV COVID-19 vaccine. His complete blood picture showed pancytopenia. A detailed infectious disease workup was unrevealing; however, his bone marrow biopsy revealed increased histiocyte activity, with some showing hemophagocytosis and dysplasia. Immunohistochemistry (IHC) profile demonstrated strong CD 68 positivity. Further investigations showed raised serum ferritin and fasting triglyceride levels. He was immediately started on dexamethasone acetate at a dose of 10 mg/m2, after which his clinical symptoms, as well as his blood parameters, improved remarkably. This is the first documented case in Pakistan.
Conclusion: The data from clinical trials support the general safety profile of inactivated COVID-19 vaccines. We endorse its mass implementation. However, we believe that robust data needs to be generated to evidence any adverse events, especially those with serious outcomes. Physicians should be aware of inactivated COVID-19 vaccine as a possible trigger for HLH and start prompt treatment, resulting in favorable outcomes.
Relevance for patients: The presentation of HLH may vary and can present in an immunocompetent patient with no underlying risk factor. HLH should be kept in differentials when a patient presents with pancytopenia with a recent history of receiving COVID-19 vaccination. Steroids play a major role in the treatment of HLH, and definitive diagnosis and early treatment improve clinical outcomes.
DOI: http://dx.doi.org/10.18053/jctres.08.202202.009
Author affilation
Aga Khan University Hospital, Karachi, Pakistan
*Corresponding author
Saqib Raza Khan
Aga Khan University Hospital, Karachi, Pakistan
Email: saqib.raza31@yahoo.com
Handling editor:
Michal Heger
Department of Pharmaceutics, Utrecht University, the Netherlands
Department of Pharmaceutics, Jiaxing University Medical College, Zhejiang, China

