-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 7 Issue 6
Risk of post-intubation cardiac arrest with the use of high dose rocuronium in COVID-19 patients with acute respiratory distress syndrome: A retrospective cohort study
Natalie Kandinata, Roshan Acharya*, Aakash Patel, Aalok Parekh, Jessica Santana, Aaron Darden, Yub Raj Sedhai, Smita Kafle, Usman Younus
Kandinata et al. J Clin Transl Res 2021; 7(6):2
Published online: October 30, 2021
Abstract
Background: Post-intubation cardiac arrest (PICA) is an uncommon complication of intubation, but numbers have risen to over 1.5 times the usual number since the Coronavirus disease 2019 (COVID-19) pandemic. Due to expert recommendations, high-dose rocuronium has become a commonly used pre-intubation neuromuscular blocking agent.
Aim: We conducted this retrospective case-control observational study with the hypothesis that high dose rocuronium was not associated with higher incidence of PICA.
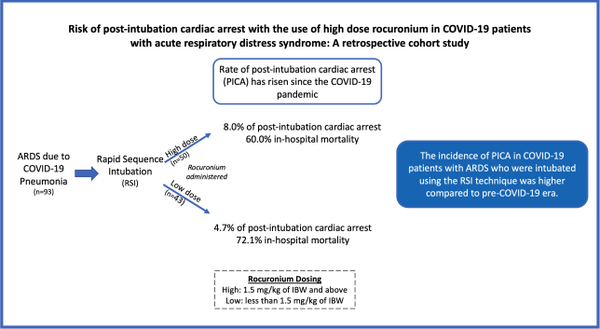
Methods: We included 93 patients who were intubated using the rapid sequence intubation (RSI) technique with rocuronium for ARDS due to confirmed COVID-19 pneumonia, admitted from March 2020 to February 2021 to a tertiary care hospital in North Carolina, USA. The patients were grouped based on high (1.5 mg/kg of ideal body weight and above) vs. low (less than 1.5 mg/kg of ideal body weight) dose rocuronium used for RSI. The differences of the various outcomes between the groups were analyzed.
Results: The baseline demographics were similar in both groups except for higher BMI in high dose group 39 vs. 32 (kg/m2), P=0.009. There was a total of six PICA events (6.45%). The high-dose rocuronium group had 8.0% of PICA vs. 4.7% in the low-dose group. In-hospital mortality was 60.0% in the high-dose rocuronium group vs. 72.1% in the low-dose group.
Conclusions: The incidence of PICA in COVID-19 patients with ARDS who were intubated using the RSI technique was higher than in the pre-COVID-19 era.
Relevance for patients: The use of high-dose paralytics during invasive ventilation with RSI and their consequences should be explored with the help of large-scale studies. The rate of PICA is still very low, and perhaps the use of high-dose rocuronium is safe, as suggested by the expert panel.
DOI: http://dx.doi.org/10.18053/jctres.07.202106.002
Author affiliation
1. Department of Internal Medicine, Cape Fear Valley Medical Center, Fayetteville, NC, 28306
2. Department of Internal Medicine, Campbell University School of Osteopathic Medicine, Buies Creek, NC, 27506
3. Department of Respiratory Therapy, Cape Fear Valley Medical Center, Fayetteville, NC, 28306
4. Department of Internal Medicine, Virginia Commonwealth University School of Medicine, Richmond, VA, 23970
5. Bachelor of Science in Nursing, Fayetteville State University School of Nursing, Fayetteville, NC, 28301
6. Department of Critical Care Medicine, Cape Fear Valley Medical Center, Fayetteville, NC, 28306
*Corresponding author
Roshan Acharya
Cape Fear Valley Medical Center, Campbell University Jerry M. Wallace School of Osteopathic Medicine, 1638 Owen Drive, Fayetteville, North Carolina, 28304, United States of America
Email: roshan.ach@gmail.com; racharya@capefearvalley.com
Handling editor:
Michal Heger
Department of Pharmaceutics, Utrecht University, the Netherlands
Department of Pharmaceutics, Jiaxing University Medical College, Zhejiang, China

