-
Home
-
About JCTR
-
Gold Open Access
-
Issues
-
Editorial board
-
Author guidelines
-
Publication fees
-
Online first
-
Special issues
-
News
-
Publication ethics
-
Partners
-
Submit your manuscript
-
Submit your review report
-
Editorial Office
-

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. ISSN print: 2382-6533 ISSN online: 2424-810X
Volume 7 Issue 5
A review of the presentation and outcome of sarcoidosis in COVID-19
Lina James George, Anil Mathew Philip, Kevin John John, Anu Anna George, Jemimah Nayar, Ajay Kumar Mishra, Amos Lal*
George et al. J Clin Transl Res 2021; 7(5):4
Published online: September 27, 2021
Abstract
Background: In the setting of the current pandemic, concerns have arisen regarding the multisystemic involvement of sarcoidosis and the possible exacerbations in response to the exposure to severe acute respiratory syndrome coronavirus 2 virus(SARS-CoV-2).
Aim: This study aims to compare the differences in clinical presentation, management, and outcome of COVID-19 between patients with sarcoidosis and those in the general population.
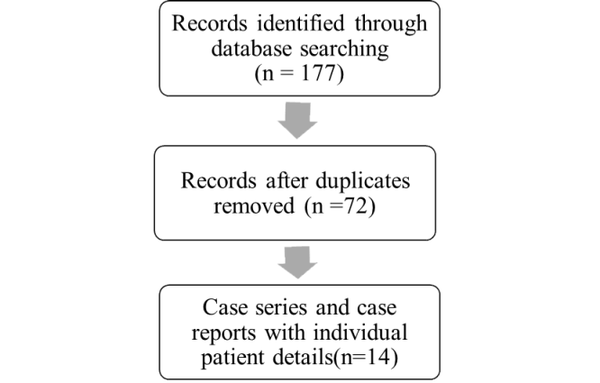
Methods: A literature search was conducted by reviewing original research articles such as case reports, case series, observational studies, and questionnaire-based surveys published in Pubmed/Medline, Web of Science, and google scholar. Data from individual patients in case series and case reports have been pooled to create a data set that was compared with larger such cohorts obtained from several other observational studies.
Results: 27 patients were identified from 14 original articles. No significant differences were found in the clinical manifestations of patients with sarcoidosis presenting with COVID-19 as compared to the general population. The rate of hospitalization in our study was found to be 48.1%. The overall mortality in our study was 7.4%, which is higher than the global average of 2.1%.
Conclusion: Our observations have reinforced the hypothesis that the presence of additional medical comorbidities is associated with a higher risk of ICU admission. Furthermore, the presence of moderate to a severe limitation in pulmonary functions is an additional risk factor associated with increased hospital admissions and mortality in sarcoidosis. However, neither the diagnosis of sarcoidosis nor ongoing treatment with steroids, methotrexate, or other immunosuppressants was associated with a poorer prognosis in patients with sarcoidosis.
Relevance for patients: Patients with sarcoidosis must take added precautions to mitigate the risk of acquiring COVID-19 infection in view of the COVID-19-related mortality rate in this group of patients. Specifically, immunocompromised patients (on immunomodulator drugs and high dose steroids) have been found to have an increased risk of contracting COVID-19. Overall impact on prognostication and outcome in cases requiring hospitalization remains yet to be determined.
DOI: http://dx.doi.org/10.18053/jctres.07.202105.004
Author affiliation
1. Department of Pulmonary Medicine, DR KM Cherian Institute of Medical Sciences, Kallissery, India.
2. Department of Medicine, St. Thomas Mission Hospital, Kattanam, India.
3. Department of Critical Care, Believers Church Medical College Hospital, Thiruvalla, Kerala, India.
4. Department of Internal Medicine, Saint Vincent Hospital, Worcester, Massachusetts, USA 01608.
5. Department of Nuclear Medicine, Christian Medical College, Vellore, India.
6. Department of Internal Medicine, Division of Cardiology, Saint Vincent Hospital, Worcester, Massachusetts, USA 01608.
7. Department of Medicine, Division of Pulmonary and Critical Care Medicine, Mayo Clinic, 200 1st St SW, Rochester, MN 55905, United States.
*Corresponding author
Amos Lal
Department of Medicine, Division of Pulmonary and Critical Care Medicine, Mayo Clinic, 200 1st St SW, Rochester, MN 55905, United States.
Email: Lal.Amos@mayo.edu
Handling editor:
Michal Heger
Department of Pharmaceutics, Utrecht University, the Netherlands
Department of Pharmaceutics, Jiaxing University Medical College, Zhejiang, China

